What is H. Pylori bacteria and Why It is Tough to Tame.
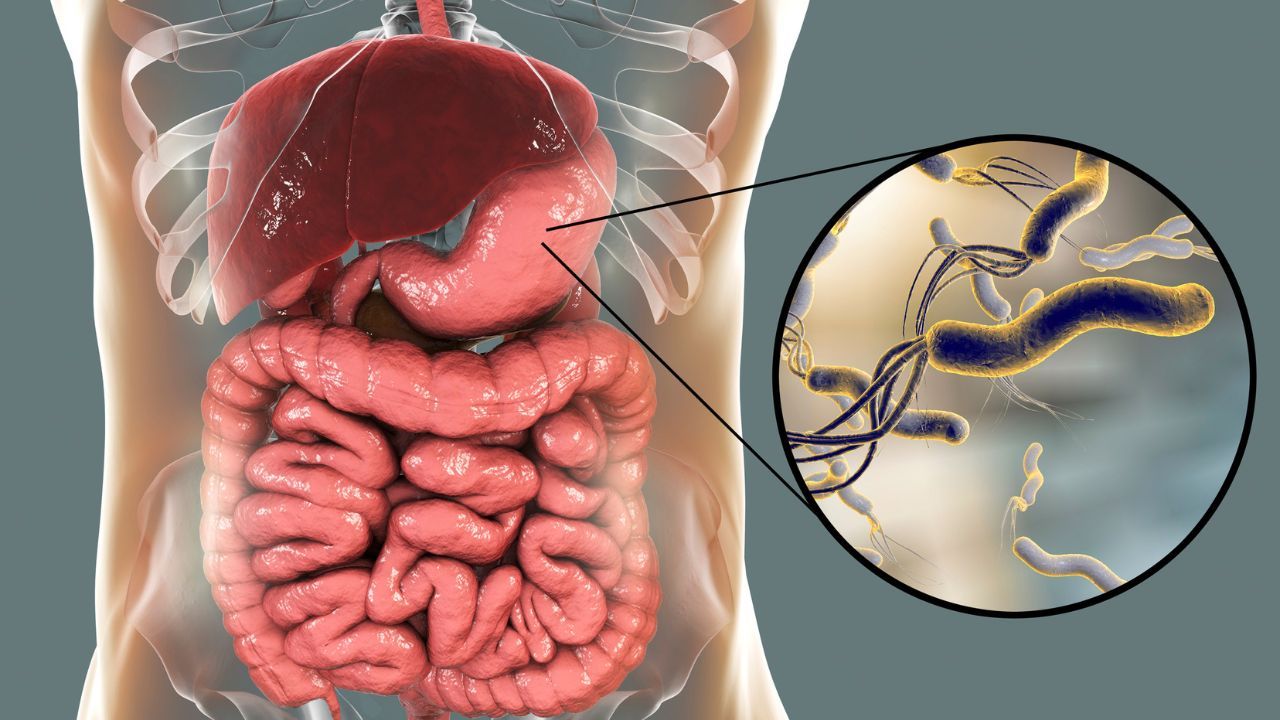
Helicobacter pylori or H. pylori is a pesky bacteria that really likes setting up shop in our stomach and can cause many problems. It’s pesky because it burrows into the stomach wall with its corkscrew tail and creates inflammation. It also promotes a likely already low stomach acid level; remember optimal amounts of stomach acid is our friend. These conditions support further gut imbalance and problems with gut integrity; especially if it overgrows which it likes to do.
As with most living organisms, especially pathogens, their end game is to survive. It does this if it has an opportunity and a favorable environment in its host - us. In other words, it happens when there is an imbalance leaving us vulnerable to infection. More importantly, if this imbalance is not healed, it will become more difficult and may feel next to impossible to keep this problematic bacteria at bay and invite even more gut microbiome imbalance.
How does H. Pylori spread?
H. pylori is usually passed between people via saliva - this can include kissing, sharing food, drink, utensils. It can also be transmitted from contaminated food or water. It’s more common in developing countries where adequate hygiene is tougher to achieve. It’s very common for many family members to have it and to continue to pass it to each other in a round robin fashion.
H. Pylori is prevalent.
How prevalent? It’s estimated that about 50% of the world’s population is colonized with h. Pylori. Colonization means that the bacteria is present but it’s not causing any symptoms or more importantly an immune response. So much so that many providers consider a finding benign if there aren't any associated symptoms. It can most certainly be considered endemic and even “friendly” if present but not necessarily overgrown. It really does come down to a person’s bio-individuality looked at through a functional lens with other points of interconnectedness. It’s also worth noting that the older you get, the higher the incidence of h. Pylori is as natural changes that occur with aging and the GI tract make infection more favorable.
I’d say that many actually do have symptoms and their immune system is responding but they don’t know it or link their symptoms to H. Pylori.
80% of all ulcers are caused by h. Pylori - actually caused by it. We have an Australian physician to thank for this who truly used himself as a guinea pig to test this hypothesis and came up very much supporting it by developing an ulcer. Don’t worry, he implemented his research and used antibiotics to get rid of the infection and ultimately healed his ulcer. At the time he was trying to teach other physicians that the cure would be antibiotics but they were dismissive because it was thought that ulcers were due to emotional/mental stress. This is significant as it shows how an infection can skew the immune system ultimately burdening it so much that the cells mutate into cancer.
It’s also significant because it supports that science is always evolving; it’s never fixed.
What are some symptoms of H. Pylori?
- Acid reflux, GERD or gastritis
- Gnawing discomfort or pain in the stomach area, especially just after eating
- Upper abdominal bloating with a sense of fullness, especially just after eating
- Skin issues such as acne
- Hair loss
- Fatigue
- Trouble sleeping
- Mood issues such as anxiety and dysthymia - a low level depression where you struggle with joy and motivation
Yup, H. pylori is linked to many extra gastrointestinal or outside the gut symptoms such as the ones above. It not only can cause GI symptoms but its cascade of damage including inflammation, hypochlorhydria, dysbiosis can cause all sorts of nutrient deficiencies which lead to low vitamin, neurotransmitter and hormone production that can affect everything from sleep, mood and energy to skin and autoimmune connections. There’s also data to link h. Pylori with certain autoimmune illnesses such Hashimoto’s thyroiditis.
It’s hard to believe that a very common bug can be so problematic. It can be difficult to tame for a few reasons but nervous system regulation is paramount to be successful at maintaining gut microbiome balance.
Benefits to H. Pylori?
It is worth noting that as more functional research develops around h. Pylori, there are some theories that h. Pylori can be somewhat protective against more virulent bacteria or immune dysregulation. For example, this can be seen in people who have asthma or autoimmune illnesses. It really requires a deep dive into a specific person and their imbalances and points of interconnectedness.
The root of this imbalance is usually our nervous system. We must be appropriately in a rest, digest and repair state to heal from anything. Most of us are far from that. We are chronically stressed either emotionally or physically. More on that a little later but here are some highlights about the actual bacteria.
How do you know if you have H. Pylori?
If you are experiencing any of the above symptoms, your healthcare provider can test you. A heads up though, they may not see any association between h. Pylori and sleep troubles but I assure you they exist. Here’s how you can be tested:
- A stool antigen test - this tests for acute infection via your stool
- A breath test - this also tests for acute infection via your breath to detect urea which is produced when h. Pylori is present
- Pathology via an endoscopy - a gastroenterologist will usually take a sample of tissue when doing this procedure as most seek this care and will have some symptoms associated with h. Pylori. It’s sent to the lab for analysis of h. Pylori presence
- A comprehensive stool test - there are a few but using a PCR based test can be a great tool to not only see actual levels of its presence but it can show many other types of dysbiosis that often co-occur. It also gives insight and data points on the health of your digestion, mucosal immunity and inflammation and gut lining.
If you’ve had h. Pylori in the past, you will have likely developed an antibody which can be measured via your blood. This doesn’t show if there’s an acute infection. If it is negative and no antibody has been detected, then h. Pylori is likely not an issue for you.
It’s important to discuss the best way to assess your h. Pylori status with your personal healthcare provider as there are some caveats to each test such as if you are taking stomach acid suppressing medication or a smoker.
How can you treat it?
Most conventional healthcare will treat it with a couple different antibiotics at the same time and a medication to suppress stomach acid production while treatment is in progress. It’s worth noting that there is a high antibiotic resistance rate so antibiotic choices may not work. Treatment duration is usually about two weeks.
There are multiple herbal antimicrobials that can be used instead that are a bit gentler but equally if not more effective. Duration of treatment is a bit longer at about 6 weeks but this also gives time for someone to peek into their lifestyle and cultivate self awareness and see where they are at - especially where their nervous system is at. Time can be your friend.
Neither way is wrong. In fact, each may have its benefits depending on certain factors such as level of infection, symptoms and other imbalances. It’s always important to speak to your healthcare provider or work with a well versed practitioner to help guide you.
It’s equally important to test and/or treat family members to prevent repeat infection or overgrowths.
How do you know it’s been treated adequately?
You can always opt to test again about 6-8 weeks after completion of therapy. You will also likely see signs and symptoms improve.
Here is the most important take away:
Start managing your stress. Whether it be emotional/mental or physiological such as other chronic illnesses, their impact is inhibiting you from getting well.
No matter what treatment you decide on, if you are not in a rest, digest and repair state the very vast majority of your time where you are calm, sleeping well, well nourished, detoxing optimally, you will not heal. Ever.
There are practitioners out there, like us, to guide you in healing. You never have to go it alone.
All it takes is reaching out. It is our biggest honor to help guide you.
Is chronic bloating a regular part of your life? Well it doesn't have to be.
Chronic bloating may be common, but it is NOT normal!
Bloating itself isn't the problem, it's usually a sign that something deeper is going on. Watch this free one hour masterclass and learn the 4 main types of bloating, their causes and what you can do to become bloat free for good!

